This week in the BMJ
Volume 328,
Number 7436,
Issue of 14 Feb 2004
![[Down]](/icons/down.gif) Practice based education increases delivery of preventive health care to children
Practice based education increases delivery of preventive health care to children
![[Down]](/icons/down.gif) Statin use varies across Europe and is on the increase
Statin use varies across Europe and is on the increase
![[Down]](/icons/down.gif) Identifying excessive mortality depends on test used
Identifying excessive mortality depends on test used
![[Down]](/icons/down.gif) Does intraoperative death affect surgeons' subsequent practice?
Does intraoperative death affect surgeons' subsequent practice?
![[Down]](/icons/down.gif) Introducing Dr Foster's case notes
Introducing Dr Foster's case notes
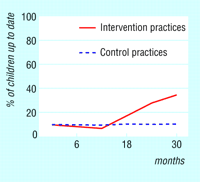
Practice based education increases delivery of preventive health care to children
Practice oriented education combined with better process methods improves rates of delivery of preventive care to children in primary care. Margolis and colleagues (p 388) conducted a randomised controlled trial among 44 private paediatric and family practices in North Carolina and found that, one year later, the practice based education group had a four times larger proportion of children receiving age appropriate immunisations and screening for anaemia, tuberculosis, and lead. The authors say that further studies should evaluate the costs and reliability of this intervention.
![[To top]](/icons/back.gif)
Statin use varies across Europe and is on the increase
Stains are widely used in Europe, but inconsistently across the continent. Walley and colleagues (p 385) surveyed administrative data and report that the variations in the incidence of coronary heart disease do not explain all the differences in use of statins across countries. They suggest that political and cultural factors also play a part. For example, the participation of doctors in clinical trials in Norway spurred the use of statins in that country, whereas the lag in reimbursement of statins in Denmark slowed their uptake in that region. The authors say that the rapid increase in use is due to growing recognition of the effectiveness of statins, an emphasis on prevention of heart disease, and successful marketing strategies by the manufacturers.

| |
Credit: PHANIE/REX
|
|
![[To top]](/icons/back.gif)
Identifying excessive mortality depends on test used
When to sound the alarm on a high death rate depends on the method used to detect it. Poloniecki and colleagues (p 375) compared the mortality among heart transplantation patients at St George's Hospital, London, with a benchmark death rate using seven different methods. They found that each gave a different answer as to whether and when the death rate of the transplant programme was excessive. Overall, the average mortality, sequential probability ratio, and cusum tests indicated a death rate higher than benchmark, whereas the remaining four tests yielded negative results. Six of these tests found that the transplant programme had a higher than benchmark death rate at some point during its 15 year existence. The authors conclude that an above average death rate does not necessarily indicate a low quality of service and suggest that the implementation of hospital mortality monitoring groups are the best way forward.
| |
Credit: JAMIE ANDREA YANAK/AP
|
|
![[To top]](/icons/back.gif)
Does intraoperative death affect surgeons' subsequent practice?
Surgeons worry about whether they ought to continue operating immediately after an intraoperative death, but no guidelines exist on the subject. Goldstone and colleagues (p 379) investigated the attitudes and practices of cardiac surgeons and anaesthetists in the United Kingdom about intraoperative death. Firstly, they surveyed 371 surgeons and anaesthetists and found that over a quarter thought they should stop operating after an intraoperative death, and most wanted guidance. The authors then compared the outcomes of 233 patients operated on by a surgeon who had experienced an intraoperative death within the preceding 48 hours with those of controls. They found no increased mortality in operations performed in the immediate aftermath of an intraoperative death, but survivors had longer hospital stays.

| |
Credit: FRANK WALSH/PHOTONICA
|
|
![[To top]](/icons/back.gif)
Introducing Dr Foster's case notes
This week's journal features the debut of Dr Foster's case notes, our new monthly page highlighting data from Dr Foster, an independent London based organisation that analyses the availability, quality, and costs of health care in the United Kingdom and globally. We aim to provide doctors, managers, and patients with data about how various treatments and systems work in the real, messy world of clinical practice. Dr Foster uses administrative data such as hospital episodes statistics and self reported data collected from hospitals by survey. This month's Dr Foster's case notes reports that acute stroke units and early computed tomography scans are associated with lower in-hospital death rates.
![[To top]](/icons/back.gif)
Practice based education increases delivery of preventive health care to children
Statin use varies across Europe and is on the increase
Identifying excessive mortality depends on test used
Does intraoperative death affect surgeons' subsequent practice?
Introducing Dr Foster's case notes