This week in the BMJ
Volume 329,
Number 7473,
Issue of 30 Oct 2004
![[Down]](/icons/down.gif) NICE influences prescribing but has more to do
NICE influences prescribing but has more to do
![[Down]](/icons/down.gif) Evidence based training improves surfactant use
Evidence based training improves surfactant use
![[Down]](/icons/down.gif) Video assisted thoracic surgery is useful but underused
Video assisted thoracic surgery is useful but underused
![[Down]](/icons/down.gif) "Mindlines" are still preferred to guidelines
"Mindlines" are still preferred to guidelines
![[Down]](/icons/down.gif) Evidence based teaching works best at the bedside
Evidence based teaching works best at the bedside
![[Down]](/icons/down.gif) Evidence based guidance affects courts' rulings
Evidence based guidance affects courts' rulings
![[Down]](/icons/down.gif) Routine EBM staff meetings are popular and useful
Routine EBM staff meetings are popular and useful
NICE influences prescribing but has more to do
The National Institute for Clinical Excellence (NICE) aims to improve health care in Britain by promoting the use of health technologies based on research evidence. Using time series analysis, case note review, survey, and interviews, Sheldon and colleagues (p 999) conducted a national study of the institute's early recommendations and found that prescribing was particularly amenable to change. There was little evidence, however, that NICE had influenced the use of surgical procedures or medical devices.
![[To top]](/icons/back.gif)
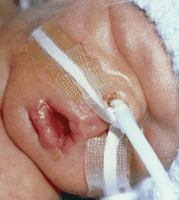
Evidence based training improves surfactant use
Training in quality improvement, comprising audit and feedback and evidence based education and support, can enhance the treatment with surfactant of preterm babies. In a cluster randomised controlled trial at 114 hospitals Horbar and colleagues (p 1004) found that, among 6039 infants of 23-29 weeks' gestation, babies in the training group hospitals received surfactant more often and sooner after birth than those born in control hospitals.
| |
Credit: GARRY WATSON/SPL
|
|
![[To top]](/icons/back.gif)
Video assisted thoracic surgery is useful but underused
Video assisted thoracic surgery is a minimally invasive approach to diagnosing and treating diseases of the lung and pleura. In a systematic review Sedrakyan and colleagues (p 1008) found that such surgery for pneumothorax and minor resections was associated with shorter length of stay in hospital and less pain with no increase in complications when compared with thoracotomy. However, the same authors found that use of this minimally invasive technology in UK specialist units varies widely (p 1011), and this seems to be explained by surgeons' preferences rather than patients' needs.
![[To top]](/icons/back.gif)
"Mindlines" are still preferred to guidelines
Doctors and nurses in general practice may still rely more on collectively reinforced, internalised, tacit guidelines ("mindlines") to guide their practice than on high quality research evidence. In an ethnographic study set in two highly regarded general practices in England over two years Gabbay and le May (p 1013) found that primary care doctors and nurses rarely accessed and used research evidence. The authors propose ways in which formal and informal professional networks could provide better evidence.

| |
Credit: DAVE KRIEGER/PHOTONICA
|
|
![[To top]](/icons/back.gif)
Evidence based teaching works best at the bedside
Teaching evidence based medicine in clinical contexts improves knowledge, critical appraisal skills, attitudes, and behaviour, whereas teaching it in the classroom improves only knowledge. Coomarasamy and Khan (p 1017) systematically reviewed studies of teaching evidence based medicine to postgraduates and found consistent evidence supporting the superiority of clinically integrated teaching.
| |
Credit: ULRIKE PREUSS/BMJ
|
|
![[To top]](/icons/back.gif)
Evidence based guidance affects courts' rulings
If slavish compliance with evidence based guidance could expose patients to foreseeable harm, such care might be considered substandard by some courts. In a clinical review (p 1024) Hurwitz discusses the impact that such guidelines might have on courts' criteria for deeming clinical care to be inappropriate or negligent. He concludes that evidence based guidelines do not set legal standards for clinical care, but they do provide courts with a benchmark by which to judge clinical conduct.

| |
Credit: ALISDAIR MACDONALD/REX
|
|
![[To top]](/icons/back.gif)
Routine EBM staff meetings are popular and useful
Introduced into London's Hospital for Tropical Diseases in 1997, routine evidence based medicine (EBM) meetings are still well attended by staff, have led to evidence based changes in hospital guidelines, and are generating topics for audit and research. Lockwood and colleagues (p 1020) summarise the effects of their seven years' experience, giving examples of meetings' outcomes, and provide advice for others who may be considering implementing such meetings.
![[To top]](/icons/back.gif)
NICE influences prescribing but has more to do
Evidence based training improves surfactant use
Video assisted thoracic surgery is useful but underused
"Mindlines" are still preferred to guidelines
Evidence based teaching works best at the bedside
Evidence based guidance affects courts' rulings
Routine EBM staff meetings are popular and useful



