This week in the BMJ
Volume 330,
Number 7482,
Issue of 8 Jan 2005
![[Down]](/icons/down.gif) Trials of gene transfer in humans need more caution
Trials of gene transfer in humans need more caution
![[Down]](/icons/down.gif) Decision makers need to judge credibility of economic evaluations
Decision makers need to judge credibility of economic evaluations
![[Down]](/icons/down.gif) Demedicalising neck pain helps patients
Demedicalising neck pain helps patients
![[Down]](/icons/down.gif) Expertise based trials may be the way forward for evaluating surgical interventions
Expertise based trials may be the way forward for evaluating surgical interventions
![[Down]](/icons/down.gif) Migraine may be a risk factor for stroke
Migraine may be a risk factor for stroke
Trials of gene transfer in humans need more caution
The public, rather than trial participants, will likely bear many of the consequences of latent risks associated with gene transfer. On page 79, Kimmelman reviews recent developments in gene transfer in humans, focusing on the risks in such clinical trials, especially for healthy trial participants. He argues that uncertainties of risks demand central ethical review of all trial protocols and emphasises that so far only the United Kingdom and Australia have implemented measures to track the health of trial participants in the long term.
![[To top]](/icons/back.gif)
Decision makers need to judge credibility of economic evaluations
Cost effectiveness assessments submitted to the technology appraisal programme of the National Institute for Clinical Excellence (NICE) by manufacturers of the relevant healthcare technologies differ significantly from those contracted by university based assessment groups. Miners and colleagues (p 65) retrospectively compared 62 appraisals. Manufacturers' estimates of incremental cost effectiveness ratios were lower (suggesting a more cost effective use of resources) than those produced by the assessment groups (25 were lower, 29 were the same, none were higher; P < 0.01).

| |
Credit: IMX/REX
|
|
![[To top]](/icons/back.gif)
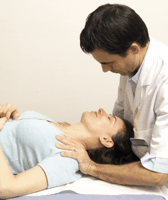
Demedicalising neck pain helps patients
Brief physiotherapy interventions focused on demedicalising the problem and teaching the principles of cognitive behaviour therapy can be as beneficial as standard physiotherapy for patients who prefer this treatment. Klaber Moffett and colleagues (p 75) randomised 268 patients to standard physiotherapy (five sessions) or up to three sessions of the brief intervention. Overall, patients who received standard care reported a significant improvement compared with patients in the brief intervention group, but patients who preferred the brief intervention and received this treatment had similar outcomes to patients receiving usual physiotherapy.
| |
Credit: A J PHOTO/SPL
|
|
![[To top]](/icons/back.gif)
Expertise based trials may be the way forward for evaluating surgical interventions
Although a randomised controlled trial is the best study design for evaluating pharmacological interventions, scepticism about whether it is best in non-pharmacological interventions (such as surgery) remains. Devereaux and colleagues (p 88) propose an alternative: the expertise based randomised controlled trial, in which participants are randomised to clinicians with expertise in intervention A or intervention B. They argue that increased use of the expertise based design will enhance the validity, applicability, feasibility, and ethical integrity of randomised controlled trials in surgery and other non-pharmacological areas.
![[To top]](/icons/back.gif)
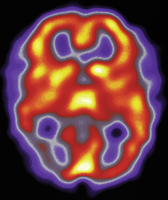
Migraine may be a risk factor for stroke
Migraine may be an independent risk factor for ischaemic stroke, and the risk is higher among oral contraceptive users and younger adults. Pooling the data from 11 case-control studies and three cohort studies, Etminan and colleagues (p 63) found that having migraines more than doubles the risk for an ischaemic stroke (relative risk 2.16, 95% confidence interval 1.89 to 2.48). The risk was greater in people who had migraine with aura than in those without aura, and was about eightfold greater in users of oral contraceptives than in those not using them.
| |
Credit: CHARING CROSS HOSPITAL/SPL
|
|
![[To top]](/icons/back.gif)
Trials of gene transfer in humans need more caution
Decision makers need to judge credibility of economic evaluations
Demedicalising neck pain helps patients
Expertise based trials may be the way forward for evaluating surgical interventions
Migraine may be a risk factor for stroke


