This week in the BMJ
Volume 330,
Number 7493,
Issue of 26 Mar 2005
![[Down]](/icons/down.gif) HIV patients need new antiretroviral drugs
HIV patients need new antiretroviral drugs
![[Down]](/icons/down.gif) Nurse led intermediate care may not be cost effective in acute hospitals...
Nurse led intermediate care may not be cost effective in acute hospitals...
![[Down]](/icons/down.gif) ... but nurse led secondary prevention clinics do seem to be cost effective
... but nurse led secondary prevention clinics do seem to be cost effective
![[Down]](/icons/down.gif) First year after diagnosis of early breast cancer is most dangerous for depression
First year after diagnosis of early breast cancer is most dangerous for depression
![[Down]](/icons/down.gif) GP registrar recruitment should be based on competence
GP registrar recruitment should be based on competence
![[Down]](/icons/down.gif) New diagnostic tests need more rigorous evaluation
New diagnostic tests need more rigorous evaluation
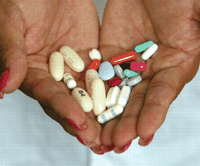
HIV patients need new antiretroviral drugs
Some HIV infected patients taking highly active antiretroviral therapy may be in danger of exhausting their treatment options, and new drugs with low toxicity to which the virus is not resistant need to be developed urgently. In a multicentre cohort study lasting seven years and including 16 593 patients in southeast England, Sabin and colleagues (p 695) assessed the association of exposure to antiretroviral drugs, CD4 cell count, and plasma HIV RNA burden. Although patients' immunological and virological status generally improved, a small but growing proportion of patients seemed to be in danger of exhausting current treatment options.
| |
Credit: JOE RAEDL/GETTY IMAGES
|
|
![[To top]](/icons/back.gif)
Nurse led intermediate care may not be cost effective in acute hospitals...
Investment in intermediate care in community hospitals may be more cost effective than financing nurse led care for post-acute patients in acute hospitals. In a cost minimisation analysis from an NHS perspective using data from a randomised controlled trial including 238 patients, Walsh and colleagues (p 699) found that total costs at six months were on average significantly higher for nurse led care than standard care in a large teaching hospital (difference £2710, 95% confidence interval £518 to £4903), but there was no difference in patients' physical functioning or destination after discharge.
![[To top]](/icons/back.gif)
... but nurse led secondary prevention clinics do seem to be cost effective
Nurse led clinics for secondary prevention of coronary heart disease in primary care seem to be cost effective compared with most interventions in health care. In a cost effectiveness analysis of 1343 patients randomised to nurse led secondary prevention clinics or no intervention in 19 general practices in north east Scotland, Raftery and colleagues (p 707) found that, during the four year follow-up, 28 fewer patients died in the intervention group at an increased cost to primary care of £136 per patient.
![[To top]](/icons/back.gif)
First year after diagnosis of early breast cancer is most dangerous for depression
In the first year after the diagnosis women with early breast cancer are at particular risk of developing depression or anxiety and therefore need dedicated psychological interventions that focus on improving social support. In a cohort study following up 222 women after diagnosis for five years or until recurrence, Burgess and colleagues (p 702) found prevalence of clinically important depression or anxiety to be nearly 50% in the year after diagnosis; 25% in the second, third, and fourth years; and 15% in the fifth year. Risk factors associated with longer term depression or anxiety were previous psychological treatment, lack of an intimate confiding relationship, younger age, and severely stressful non-cancer life experiences.

| |
Credit: CHRISTINA PEDRAZZINI/SPL
|
|
![[To top]](/icons/back.gif)
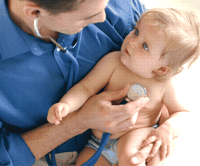
GP registrar recruitment should be based on competence
A new competency based selection system should improve the validity of selection of general practice registrars in England compared with traditional selection techniques. Through a longitudinal predictive validity study and a matched pair comparison, Patterson and colleagues (p 711) designed and validated the new selection system, which comprised competency based application form, referees' reports, and an assessment centre. Those trainees recruited through the new system performed significantly better in the job than those recruited through traditional processes.
| |
Credit: PHANIE/REX
|
|
![[To top]](/icons/back.gif)
New diagnostic tests need more rigorous evaluation
Harms and benefits of new diagnostic tests should be fully evaluated and understood before they become available for use in clinical practice, argue Gluud and Gluud (p 724). They propose a four phase process of assessment, mirroring that used for new drugs. Using brain natriuretic peptide for diagnosing heart failure as an illustrative example, they describe the four phases in diagnostic research. They claim the process is applicable to a wide range of tests including laboratory techniques, diagnostic imaging, pathology, evaluation of disability, electrodiagnostic tests, and endoscopy.
![[To top]](/icons/back.gif)
HIV patients need new antiretroviral drugs
Nurse led intermediate care may not be cost effective in acute hospitals...
... but nurse led secondary prevention clinics do seem to be cost effective
First year after diagnosis of early breast cancer is most dangerous for depression
GP registrar recruitment should be based on competence
New diagnostic tests need more rigorous evaluation



